
Healthcare organisations struggle with inconsistent metric definitions across systems, leading to reporting gaps, reduced trust and slower decisions. A semantic layer solves this by standardising definitions, entities and relationships into a governed framework. This ensures consistent reporting, improves auditability and enables reliable analytics and AI-driven insights.
Healthcare organisations are not struggling with a lack of data. They are struggling with a lack of consistent meaning. Across hospitals, insurers and care networks, key metrics such as readmission rates, length of stay and cost per case are often defined differently across systems, teams and dashboards.
This inconsistency creates more than reporting discrepancies. It erodes operational trust, introduces friction into performance management, complicates audit and compliance processes, and delays decision-making at critical moments. When leadership teams cannot reconcile numbers across reports, confidence in the underlying data breaks down.
The impact is even more pronounced as organisations scale AI and advanced analytics. Models trained on inconsistent definitions produce unreliable outputs, limiting their effectiveness and increasing risk. Without a shared semantic foundation, healthcare organisations are not just misaligned in reporting, they are constrained in their ability to operationalise intelligence at scale.
The root of the problem is not the lack of data. It is the lack of shared meaning across systems and tools. When metric logic is scattered across bespoke SQL queries or embedded in individual BI dashboards, every team ends up reinventing the same definitions in its own way. This leads to delayed quality reviews, repeated reporting rework, and frequent disputes in executive discussions over which numbers to trust. In healthcare, where quality measures are tied to regulatory reporting, financial performance, and clinical outcomes, this inconsistency carries real risk.
A semantic layer changes this dynamic. Rather than embedding metric logic in a specific report or tool, the semantic layer codifies definitions, relationships and business rules into a governed, reusable framework. In practice, this consistency is only achieved when the semantic layer is supported by high-quality source data, robust terminology governance and consistent adoption across consuming teams. It becomes the contract between data, business intelligence and AI, ensuring that all consumers interpret patients, episodes, diagnoses and performance metrics the same way.
When BI systems, analytics platforms and AI models draw from a shared semantic layer, they produce consistent, trustworthy intelligence across the organisation. The result is not simply cleaner dashboards, but a unified foundation for decision-grade insight, accelerated analytics delivery and better alignment between clinical, operational and financial stakeholders.
Healthcare data environments are rarely homogeneous. Electronic health records (EHR), claims systems, lab information systems, and cost accounting platforms all define their own structures and terminologies. Without a shared understanding of meaning, a “30-day readmission” in one system may not correspond to the same set of events in another.
Traditional models embed metric logic directly into database views or BI queries. For example, one team might define readmission based on discharge date, another based on admission date. Another team might include or exclude transfers. These definitions live in code rather than in a governed semantic layer. As a result, dashboard outcomes diverge, and reconciling them becomes a manual, time-consuming process.
A semantic layer changes this by capturing the meaning of healthcare concepts and metrics independently of any one data source or BI tool. It defines what entities represent (such as patient, encounter and diagnosis), how they relate, and how metrics are computed using explicit, governed logic. This consistency is reinforced through alignment with standard clinical terminologies and interoperability frameworks, where mappings to vocabularies such as SNOMED CT, ICD-10 and LOINC ensure that concepts are interpreted consistently across systems. The semantic layer becomes the contract that analytics, BI and AI systems rely on for consistent interpretation.
This contract is not abstract. In practice, it consists of governed metric definitions, canonical entities, standardised terminology mappings, clear data lineage and structured change control processes. Together, these elements ensure that every metric is defined, traceable and consistently applied across the organisation. Because healthcare metrics directly inform clinical decisions, financial planning, quality reporting and compliance, any inconsistency introduces risk. Without this level of semantic discipline, organisations are effectively making decisions on unstable foundations.
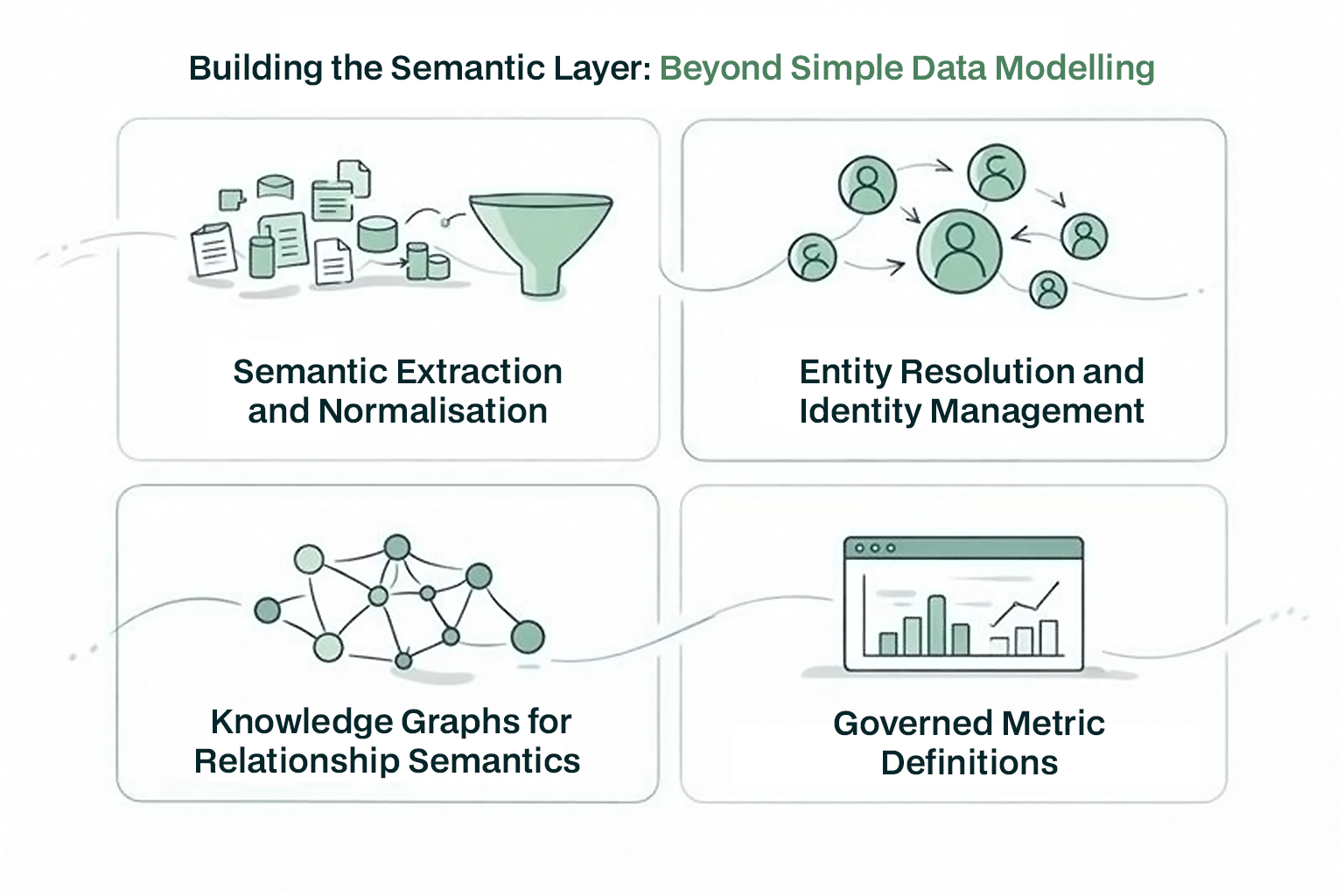
A semantic layer is more than a shared glossary or a common set of definitions. It is a structured representation of domain meaning, encoded in a way that both BI systems and AI models can consume reliably. It combines semantic modelling, terminology management, entity resolution and metric governance into a unified framework. In practice, this means it functions both as a technical architecture that standardises how data is interpreted, and as a governance mechanism that ensures definitions remain consistent, controlled and reusable across the organisation.
Merit helps organisations build this layer through a combination of technologies and practices that address key challenges in healthcare semantics:
Raw healthcare data exists in many forms: structured tables in EHRs, free text in clinical notes, PDFs in reporting systems, and semi-structured outputs from scheduling or lab platforms. Extracting meaning requires converting these diverse representations into consistent, machine-readable constructs.
Merit’s data orchestration and semantic extraction capabilities ingest these varied sources, normalise terminologies and align them with controlled vocabularies. This goes beyond simple synonym matching. Clinical normalisation depends on context, coding standards and terminology services, where concepts are mapped to established vocabularies and classification systems. For example, representations such as “MI”, “myocardial infarction” or “heart attack” are not just treated as equivalent labels, but are resolved and encoded against standard terminologies and mappings to ensure consistent interpretation across clinical, operational and reporting use cases.
Healthcare entities often appear in multiple places with different identifiers. A patient may have separate IDs in an EHR and a claims system. A provider may be referenced differently in credentialing and care delivery systems.
Merit’s entity resolution technology reconciles these identities into canonical entities that persist across systems. In practice, this resolution is often probabilistic, governed by matching policies, confidence thresholds and stewardship workflows to ensure accuracy and minimise risk, particularly in patient identity matching. This makes it possible to build metrics that reliably relate encounters, providers, diagnoses and outcomes across an organisation’s entire data estate.
Relationships matter in healthcare: an encounter is linked to a patient, a diagnosis is linked to a clinical episode, a quality measure depends on multiple events. To represent these complex relationships, Merit uses knowledge graph approaches that encode entities and their connections in a flexible, semantically rich layer.
This graph model allows BI and AI systems to traverse relationships when computing metrics or generating insights. Unlike traditional relational joins or dimensional models, a knowledge graph makes relationships, lineage and dependencies explicit and governed, rather than implicit in query logic. This makes it easier to trace how data points are connected, understand how metrics are derived, and apply consistent reasoning across complex care pathways, such as mapping diagnosis groups to quality outcomes across episodes of care.
Core business metrics in healthcare must be defined with precision. For example, the calculation of a 30-day readmission rate requires clear rules about the starting point, exclusion criteria, handling of transfers and applicable patient cohorts. When this logic is captured in BI dashboards individually, consistency erodes. Without central ownership, versioning and formal change approval processes, metric definitions can drift over time, leading to discrepancies that are difficult to trace and govern.
In a semantic layer, metric logic is captured once, documented, versioned and governed. Merit’s platforms support these metric definitions centrally so that any BI tool consuming the semantic layer retrieves the same, audited logic. This centralised governance is critical for quality reporting, regulatory compliance and internal performance management.
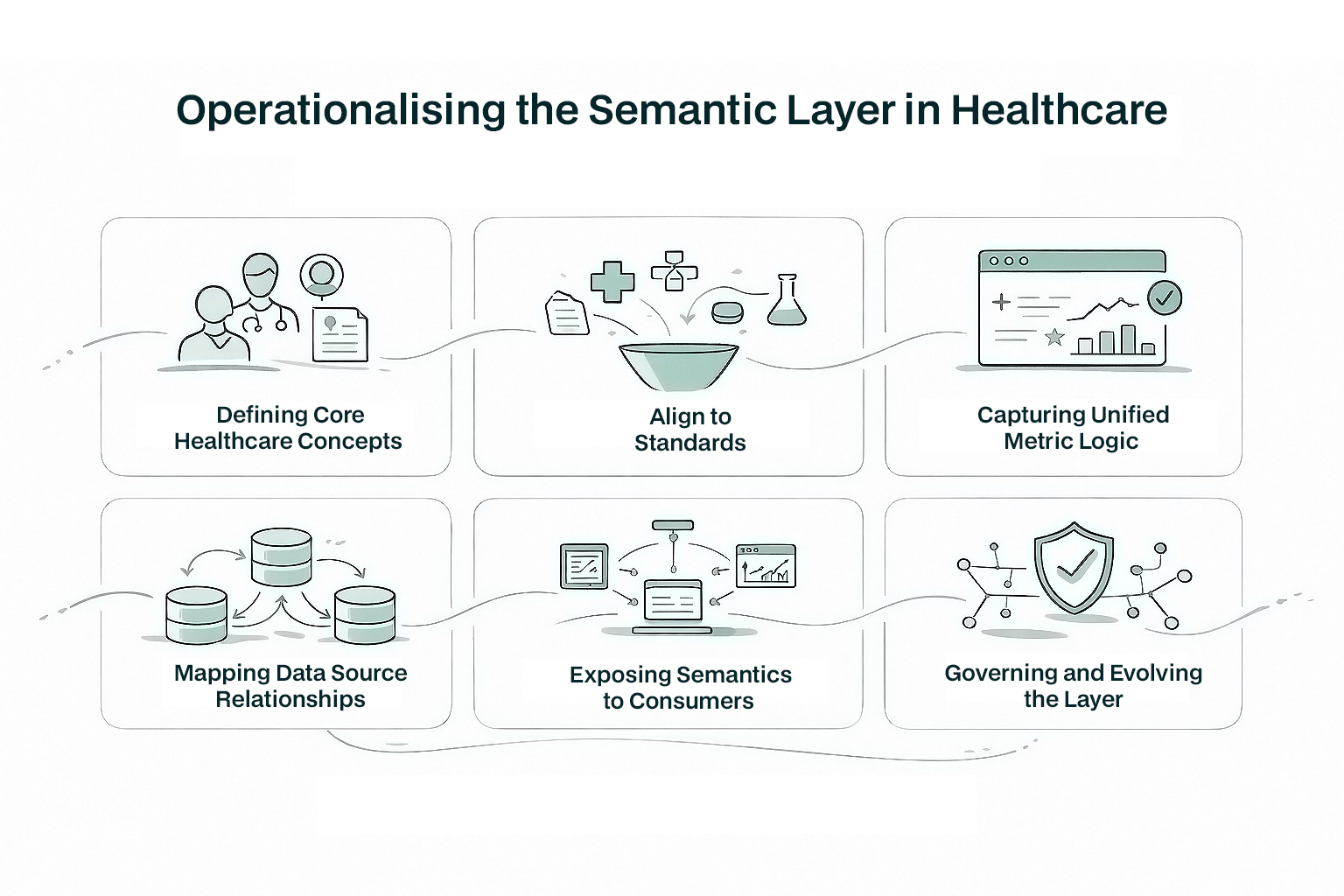
Implementing a semantic layer is not a one-off project. It is an ongoing enrichment of the enterprise data architecture that supports reuse, evolution and governance over time. In practice, organisations adopt it as an operating pattern rather than a fixed sequence, with the starting point shaped by their existing maturity in areas such as terminology governance, enterprise data modelling and quality measure management.
The first step is to agree on the core entities and their canonical representations. Clinical informatics teams, analytics experts and domain leaders collaborate to define entities such as patients, providers, encounters, diagnoses, procedures and service lines. These definitions are aligned with established standards, where SNOMED CT supports detailed clinical terminology and semantic interoperability, LOINC standardises laboratory and observation data, and ICD-10 provides classification for reporting and billing. Together, these mappings form the backbone of the semantic layer.
Merit’s extraction and normalisation capabilities assist here by identifying entity mentions across structured and unstructured data and consolidating them against defined standards.
Organisations capture metric logic in the semantic layer rather than embedding SQL in individual dashboards. Metric definitions are written once and stored in a central repository, including computation logic, filter criteria, cohort definitions, exclusions, risk adjustments and business rules. Many healthcare measures also require retrospective restatement rules to account for late-arriving data or updates to clinical records, adding further complexity to how metrics are governed.
For example, a quality improvement team may work with data engineers to codify the definition of a “risk-adjusted mortality rate” and document how it should be computed from raw encounter, diagnosis and outcome data. Once captured, this logic is available across all BI tools and analytics pipelines.
The semantic layer does not replace raw data storage. Rather, it maps logical entities and metrics to underlying data structures through defined source mappings, terminology alignment and transformation logic. This includes reconciling differences in schemas, handling schema drift over time, and ensuring that data elements from disparate systems remain consistently aligned with the semantic definitions.
Merit supports these mappings through data orchestration workflows that reconcile data structures, normalise formats and enforce consistency as new data arrives.
Once defined, the semantic layer is exposed to reporting tools, notebooks and AI systems through governed semantic services, models and metadata layers. For business users, this provides a consistent and approved way for tools such as Power BI, Tableau, Qlik and analytics platforms to consume the same definitions without ambiguity. For technical teams, this is typically enabled through structured semantic models, query layers and metadata exposure rather than generic APIs alone.
This enables reuse across tools: a measurement defined once is consumed everywhere without reimplementation.
Governance processes ensure that the semantic layer remains accurate and relevant over time. When clinical definitions change, quality standards are updated, or new reporting requirements emerge, semantic definitions are updated through controlled workflows. Stakeholders review changes, approve updates and version definitions so that historical reports remain valid and comparable.
In healthcare, this governance is critical for auditability. Organisations must be able to explain exactly how a reported measure was derived, which source elements were used, how terminology mappings were applied, and which version of the definition was in effect at the time. Differences in code mappings or interpretations across systems can introduce significant risk if not governed carefully. Merit’s metadata management and lineage tracking ensure that every metric and entity is fully traceable back to its source data, transformation logic and semantic definitions, supporting compliance, audit readiness and organisational trust.
Across healthcare organisations, semantic layers deliver tangible value when applied to specific operational challenges. The following illustrative scenarios highlight how this plays out in practice.
At a large integrated care network, the introduction of a semantic layer addressed persistent inconsistencies in utilisation metrics. Different departments had interpreted length of stay using slightly different rules, leading to repeated reconciliation cycles ahead of executive and board reporting. By standardising the definition within the semantic layer and aligning it to controlled terminology, the organisation reduced manual reconciliation effort, improved confidence in reported figures, and shortened the time required to prepare performance reviews.
A national payer analytics team used a semantic layer to standardise inputs for predictive modelling across clinical and claims data. This included creating shared definitions for features such as patient cohorts, clinical events and utilisation patterns, which were reused across models. By working from these governed, reusable inputs rather than redefining features for each model, the team reduced development time, improved consistency between model outputs, and accelerated risk adjustment and population health initiatives.
In another case, a provider organisation used a semantic layer to support quality reporting against national standards. ith centrally governed metric definitions, aligned terminology mappings and documented lineage, the organisation was better equipped to respond to audit queries by tracing reported measures back to source clinical events and applied logic. While audit resolution still depended on underlying data quality and governance discipline, the semantic layer provided the transparency and structure needed to support compliance and reduce ambiguity.
These examples illustrate that semantic layers are not theoretical constructs. They are practical enablers of trustworthy, consistent and governed intelligence across analytics and AI.
In healthcare, reliable intelligence depends on more than better visualisations or faster reports. It depends on a shared understanding of meaning that spans clinical systems, operational data stores, reporting tools and AI models. Mere data integration is not enough. The organisation needs a semantic foundation that defines what a metric stands for, how it is computed, and how it relates to other concepts across the enterprise.
Merit Data and Technology approaches semantic layers as the foundation for governed, reusable intelligence across data, BI and AI. Rather than focusing only on data integration or visualisation, Merit emphasises the creation of a consistent semantic backbone that supports both analytics and operational decision-making.
Through intelligent extraction and semantic normalisation, Merit ingests structured, semi-structured and unstructured healthcare data and aligns it to controlled vocabularies and standard representations. Entity resolution frameworks reconcile patients, providers and clinical events across systems, while knowledge graph–driven models make relationships, dependencies and lineage explicit.
This foundation enables organisations to define metrics, cohorts and business logic once, with clear ownership, versioning and governance. These definitions are then exposed through governed semantic models, ensuring that BI tools, analytics workflows and AI systems consume the same approved logic.
By combining semantic engineering with embedded governance, Merit helps healthcare organisations reduce reporting inconsistencies, improve auditability, and accelerate the delivery of decision-grade intelligence across clinical, operational and financial domains.